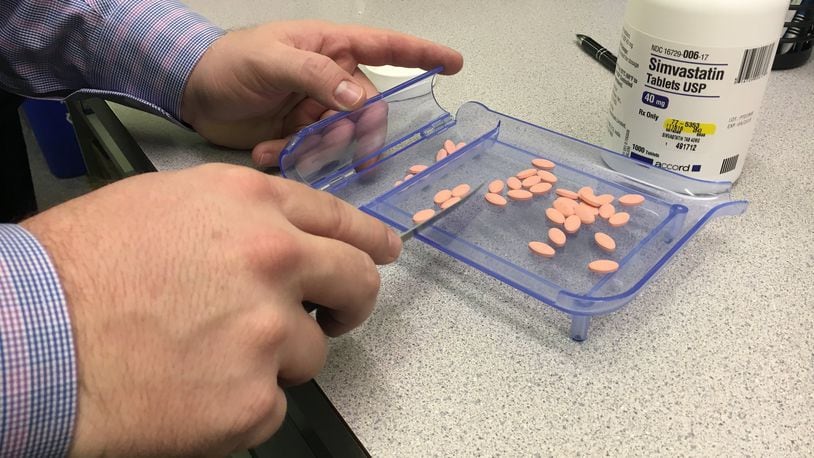
The man and other patients who get their health coverage through Anthem Inc. are suing pharmacy benefit manager Express Scripts, claiming the company schemed to inflate prescription drug prices affecting 38 million patients.
It is just the latest in a series of legal actions and accusations against the pharmacy benefit manager industry — middlemen in the prescription drug supply chain — for driving up the cost of drugs through various opaque practices.
IN-DEPTH REPORT: Read and watch the full investigation into prescription drug prices
The system for pricing prescription medication is shrouded in layers of complexity and hidden from public view, making it virtually impossible for consumers to know whether they are paying a just price at the drug counter. And because high sticker prices get spread throughout the health care system, everybody pays when prescription drugs have high markups.
Just who is to blame the skyrocketing costs is a subject of intense debate. But the legal fight between Anthem and Express Scripts has shined a spotlight on the increasing role being played by pharmacy benefit managers, who now wield power over many aspects of the prescription world, from how much drugs cost and which ones are covered or excluded by health plans to the very pharmacies patients are allowed to use.
The role of pharmacy benefit managers, or PBMs, has grown by leaps since the 1970s, when health plan sponsors began contracting with these companies as claims processors. Contrast that with today, where three PBMs control prescription benefit coverage for about 70 percent of insured individuals in the United States.
RELATED: Who's in control of your drug prices? 5 things to know
RELATED: $180,000 price tag for Miami Twp. boy's prescription
“When you have an industry of that size, that grew $80 billion over the last two years from basically about $300 billion to $380 billion, to me it should be a front page story every single day,” said Kyle Fields, president of Waynesville pharmacy benefit management company ApproRX.
Part of the reason the role of pharmacy benefit managers is obscured is so few members of the public understand how the system works. And those in the industry have wildly different opinions about whether PBMs are good or bad for the consumer. The following information should give you a better sense of how drug prices are set and help you determine whether you are paying too much.
The argument for PBMs
The giant companies that form the PBM industry say they provide huge benefits for the consumer. Here’s how:
- Leverage. With their millions of patients, PBMs can negotiate rebates from drug makers in exchange for offering a manufacturer better placement on the formulary that says which drugs are covered by the health plan and which are not. The PBM industry says the rebates save employers about 30 percent annually on their prescription drug costs.
- Competition. PBMs say their negotiations drive competition because they are able to use their immense size to the advantage of their customers. Express Scripts represents 85 million members of 3,000 different health plans, according to spokesman Brian Henry. "(We're) able to pit drug companies against each other," he said. "Like anything else in the marketplace, you're better off when there's competition."
- Improved patient care. PBMs employ physician panels to help create drug formularies they say favor the drugs with the best outcomes for patients at the lowest price.
- Exclusion lists. PBMs says they stand up to Big Pharma by refusing to cover higher-priced drugs when there are cheaper competitors of the same quality.
- Online pharmacies. Express Scripts and others own mail-order pharmacy businesses that are often cheaper and offer more convenient options for patients. They say automation has cut down on pharmacy errors which can be deadly.
The argument against PBMs
Critics of the tactics used by pharmacy benefit managers include pharmacists, patient advocacy groups and even some other pharmacy benefit managers. They say PBM pricing practices and a lack of transparency are driving up costs and causing insurers to pay inflated prices without knowing it — eventually passing those costs on to their members.
» NEWS IN YOUR INBOX: Sign up for our email newsletters on the topics you love
» EXCLUSIVE CONTENT: Download our apps for real-time alerts on the news that’s important to you
The rebates themselves are controversial, and some argue that they result in no savings to the consumer because manufacturers simply factor rebates into the price they charge for the drug. PBMs have also been accused of keeping an undisclosed amount of the rebates they negotiate while offering their clients a much smaller cut.
Many PBMs also collect a “spread” on each prescription that gets processed. If a pharmacy charges $40 for a prescription, the PBM would actually bill the health plan $40 plus 5 percent, and keep the difference.
The pharmacy benefit managers argue the rebates and spread pricing are written into the contracts signed by PBMs and their clients. But critics say it can be difficult for health plan sponsors to determine how much the pharmacy paid or how much a rebate was worth, thereby obscuring whether or not they are getting the best deal.
The rebates the big PBMs negotiate are “the best kept secret in health care,” said Antonio Ciaccia, director of Government and Public Affairs for the Ohio Pharmacy Association.
READ MORE: EpiPen prices anger parents
“Any time you have any marketplace where there are layers of people in the middle and the transactions within are not transparent, then you’ve got an arbitrarily inflated price waiting to happen,” added Kevin Schlotman, CEO of Benovation Healthcare, a third party health plan administrator based in Cincinnati.
PBMs have also come under fire for their exclusion lists, which they argue is a good tool for punishing manufacturers who over-inflate the cost of their products. But Adam Fein, who writes about the industry’s complexities on his Drug Channels blog, says it is impossible to know whether a PBM plays favorites with whoever gives it the biggest rebate.
“We can’t assess the true economic impact of exclusion lists,” he said in an August blog post. “The PBMs can claim to be standing up to pharma on behalf of payers, regardless of the actual dollar or patient impact.”
Critics also question the motives of PBMs, who often make a percentage of a drug’s list price.
“You start getting into the questions of, ‘if I’m a pharmacy benefit manager, and my compensation is better if patients have more expensive drugs, am I disincentivized from making sure people are gravitating toward lower-cost drugs?,’” Schlotman said. “There’s a potential conflict of interest there.”
RELATED: Trump: Drug companies 'getting away with murder'
But both Express Scripts and the PBM trade group Pharmaceutical Care Management Association say PBMs make more money when prices are lower because they can attract more clients. Prices are 100 percent controlled by the manufacturers, according to the PBM industry.
“It would be better for everyone if drug companies just offered lower prices,” said Mark Merritt, president of PCMA. “To try and blame PBMs for high drug prices would be like Sony raising the price of televisions and then blaming it on Walmart’s discounting practices….It just doesn’t make any sense.”
Which side is right?
Whether PBMs are giving their clients the best deal or not ultimately depends on what the contract says. And health plan experts say employers need to be more savvy in asking about rebates and spread pricing when negotiating those contracts.
“I’m not opposed to someone who brings great value to my clients getting paid, and getting paid well,” said Schlotman, whose company customizes health care plans for employers. “There’s a difference between getting paid well and getting paid a bunch of money that nobody knows about.”
Schlotman offered this scenario to show how employers can work to get the best deal possible from their pharmacy benefit managers. A PBM may offer an employer a discount on their administration fees, say $5 a month per employee. With 300 members, that’s a savings of $18,000. But by asking more questions the employer may discover the PBM received a rebate from the manufacturer for $75,000. That information can then be used when negotiating the next contract.
VIDEO GUIDE: How do drug prices get set?
Marc Sweeney, founding dean of the School of Pharmacy at Cedarville University and a health benefits consultant, said there is no blanket statement to say which side in the debate over pharmacy benefit managers is right.
“Across every drug everyone is getting gouged, that’s not a true statement. Across every drug (PBMs) are actually helping reduce cost, well that’s not a true statement,” he said. “On some drugs they are helping reduce cost and in other cases they’re not.
“If you go to the patient level I know there’s a lot of frustration because patients have to deal with chronic conditions, and people are making decisions whether or not to purchase food in some cases because they’re trying to afford medication.”
Marsha Thomas, 64, of Forest Park in Cincinnati, is one of those frustrated patients. She was diagnosed with Multiple Sclerosis in 2002, prompting her to retire from 30 plus years of nursing and go on Social Security disability. After her husband died, she no longer qualified for Medicaid, even though she only gets $1,700 in SSDI.
Thomas has had medications with list prices that range from $2,600 to $5,600 a month.
In some situations she’s been able to get patient assistance grants. But trying to scramble and find that funding when a PBM renegotiates its rebates and a medication is suddenly not covered is near impossible, she said.
“This is so confusing for me,” Thomas said. “I can’t imagine someone who has no medical background.”
MORE: Read and watch the full investigation into prescription drug prices
About the Author